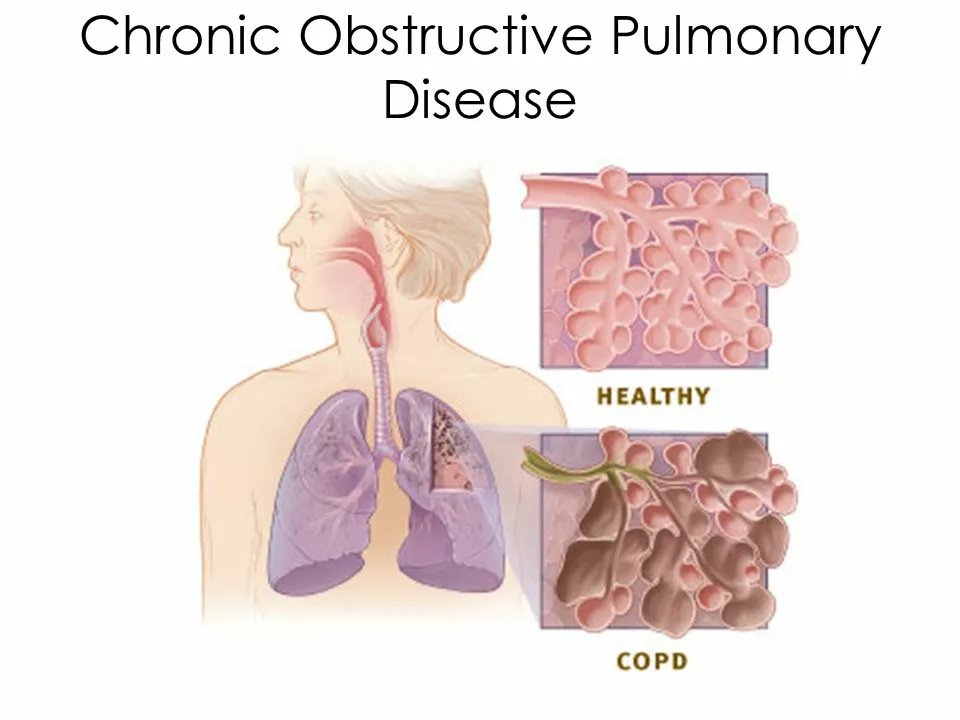
COPD: What It Is and How to Manage It
COPD stands for chronic obstructive pulmonary disease. It slowly narrows your airways and makes breathing harder over time. Most people with COPD notice long-term cough, more mucus, shortness of breath during activity, and frequent chest infections. Smoking is the main cause, but long-term exposure to dust, fumes, or indoor pollution can also trigger it.
Quick treatment guide
Treatment aims to relieve symptoms, slow lung damage, and prevent flare-ups. Your doctor will usually prescribe two types of inhalers: a short-acting rescue inhaler for sudden breathlessness (for example, albuterol) and a maintenance inhaler to keep airways open daily (long-acting bronchodilators like tiotropium, salmeterol, or formoterol). Some people also use inhaled corticosteroids or combination inhalers such as budesonide/formoterol. For severe cases, doctors may add pills like roflumilast or recommend supplemental oxygen.
Proper inhaler technique matters more than you think. Use a spacer with a metered-dose inhaler if you struggle with timing. Rinse your mouth after steroid inhalers to lower the risk of thrush. Keep an action plan so you know what to do during a flare-up and when to call your doctor—early treatment can stop a bad episode from getting worse.
Daily habits that help
Quit smoking. It’s the single most effective step to slow COPD progression. Avoid smoky places and strong fumes, and check air quality before going outside. Get seasonal flu and pneumococcal vaccines to reduce infection risk. Join pulmonary rehab if you can — it combines exercise, breathing training, and education to improve your stamina and confidence.
Use simple breathing tricks at home: pursed-lip breathing (inhale slowly through your nose, blow out through pursed lips) helps lower breathlessness during activity. Diaphragmatic breathing strengthens your breathing muscles when practiced regularly. Stay active with short, regular walks or prescribed exercises; even small improvements in fitness cut breathlessness.
Know the red flags: increased shortness of breath, rapid breathing, high fever, chest pain, blotchy or blue lips, sudden confusion, or swelling in the legs—seek urgent care. Keep a list of current meds, allergies, and your inhaler schedule in case you need to visit the ER.
Finally, talk openly with your healthcare team. Ask about inhaler technique, rehab options, and strategies to manage anxiety linked to breathlessness. With the right meds, habits, and a clear plan, most people with COPD can feel better and stay more active every day.