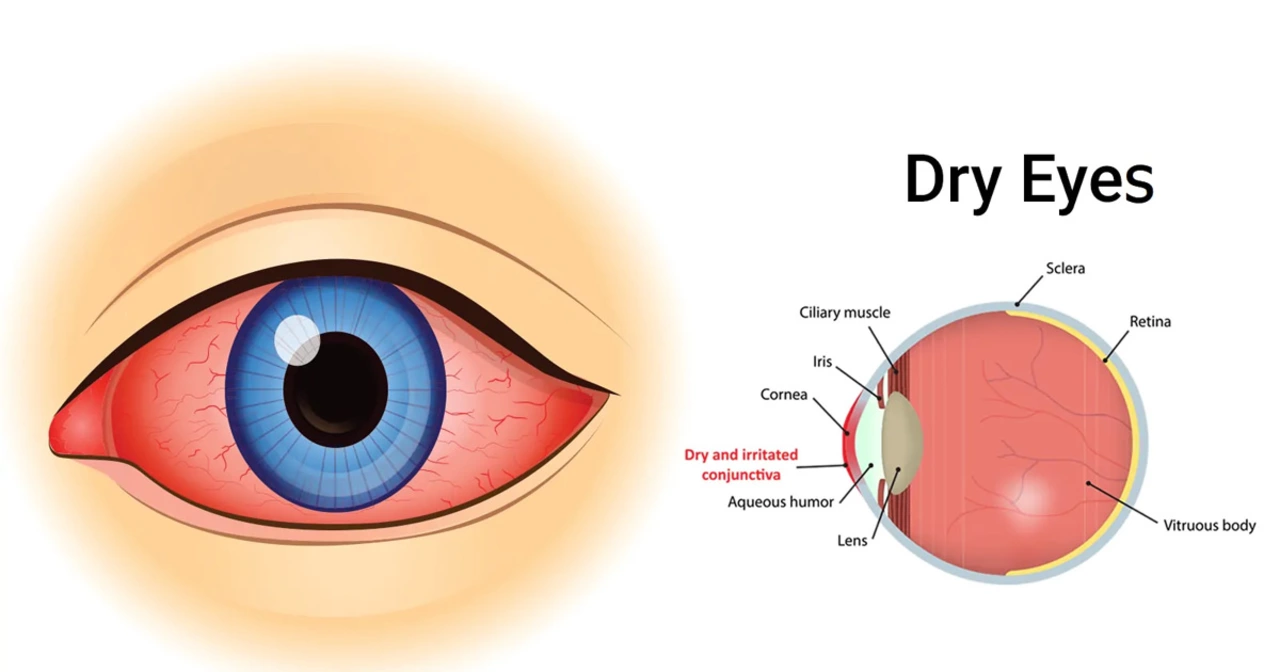
Chronic Dry Eye: What’s Really Causing Your Watery, Scratchy, or Burning Eyes
Waking up with gritty, sore eyes or feeling like you swallowed sand after staring at a screen? That could be chronic dry eye. This isn’t just occasional dryness — it’s a repeating problem that interferes with work, sleep, or comfort. The good news: most causes are manageable once you know what’s going on.
Causes and how doctors check it
Chronic dry eye has a few common reasons. One is meibomian gland dysfunction (MGD) — your eyelid oil glands get clogged and stop making the oily layer that prevents tears from evaporating. Another is low tear production, which can be linked to aging, certain medications (antihistamines, antidepressants), or autoimmune diseases like Sjögren’s. Environmental factors — dry rooms, air conditioning, and lots of screen time — make it worse.
Eye doctors diagnose this with quick, office tests: tear breakup time (how fast tears evaporate), the Schirmer test (measures tear production), and meibography (images of the oil glands). These tests show whether the problem is evaporation, low production, or both — and that determines the treatment plan.
Treatments that actually help — and smart daily steps
Start with simple, reliable moves: use preservative-free artificial tears during the day and a thicker ointment at night if you wake up stiff. Warm compresses and gentle lid massage help unclog meibomian glands. For people with heavy screen use, follow the 20-20-20 rule: every 20 minutes, look 20 feet away for 20 seconds and blink fully.
If lid hygiene and drops don’t cut it, there are proven medical options. Prescription eye drops like cyclosporine (commonly known by brand names) or lifitegrast reduce inflammation and can boost tear production over weeks. For MGD, dermatologic-dose doxycycline or azithromycin ointment can help reduce gland inflammation. Punctal plugs (tiny plugs placed in tear ducts) keep tears on the eye longer and work well for many people.
For severe cases, your specialist may suggest autologous serum drops (made from your blood) or scleral contact lenses that protect the surface while trapping moisture. Also consider a humidifier at your desk, sunglasses outdoors to block wind, and reviewing current meds with your doctor — some drugs make dry eye worse.
One common question: do supplements help? Evidence is mixed. Large trials like the DREAM study found little benefit from omega-3 supplements for dry eye, so supplements aren’t a guaranteed fix but might help some people.
If symptoms are getting worse, your vision is changing, or you have intense pain or light sensitivity, see an eye specialist. Chronic dry eye can usually be controlled, and the right mix of lifestyle changes, over-the-counter care, and targeted medical treatment will make your eyes feel a lot better.