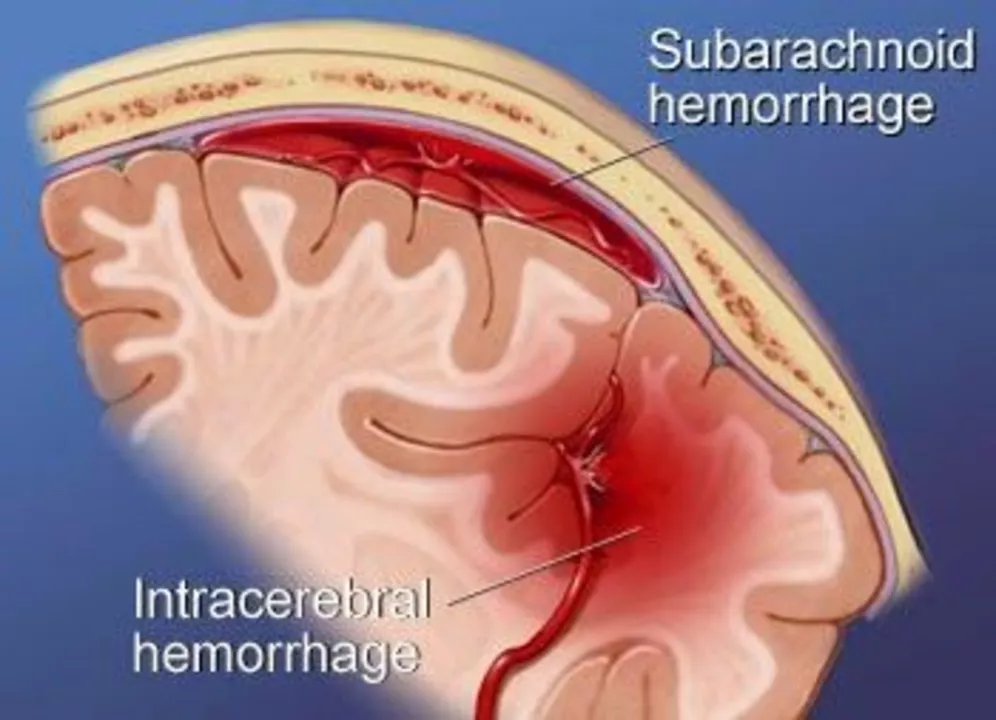
Subarachnoid Hemorrhage: What to Watch For and What to Do
If someone says they have the "worst headache of their life," take it seriously. A subarachnoid hemorrhage (SAH) is bleeding into the space around the brain. It often comes on suddenly and can be life-threatening. Knowing the signs and quick steps can make a real difference.
Recognizing the Signs
The most common symptom is a very sudden, severe headache — people describe it as a thunderclap. Other clues: neck stiffness, nausea or vomiting, sensitivity to light, drowsiness, confusion, or loss of consciousness. You might also see weakness, trouble speaking, or seizures. If symptoms follow a head injury, assume bleeding until proven otherwise.
Not every bad headache is SAH, but these features raise concern: instant peak pain, a worsening pattern over minutes to hours, or neurologic changes (slurred speech, one-sided weakness, vision changes). If you’re unsure, treat it as an emergency.
Immediate Steps: What You Can Do
Call emergency services right away. Keep the person still and calm. If they’re awake, help them lie down with their head slightly elevated. Don’t give anything by mouth if they’re drowsy or vomiting. Avoid aspirin, ibuprofen, or other blood thinners unless a doctor says so. If they stop breathing or lose a pulse, start CPR if trained.
When ambulance crews arrive, they’ll start stabilizing vital signs and getting the patient to a hospital equipped for neuro care. Time matters: early treatment lowers the risk of rebleeding and other complications.
At the hospital, doctors use a non-contrast CT scan first. If CT doesn’t show clear bleeding but suspicion remains high, a lumbar puncture or CT angiography helps find blood or an aneurysm. Once SAH is confirmed, teams focus on preventing rebleed, managing blood pressure, and watching for vasospasm (narrowing of brain vessels that can cause stroke several days after the bleed).
Treatment options include endovascular coiling (threads and coils placed via blood vessels) or surgical clipping of an aneurysm. Which one depends on the bleed’s cause, location, and the patient’s condition. Patients usually need ICU-level care, often with nimodipine to reduce the risk of vasospasm and close neurologic monitoring.
Recovery varies. Some people recover well with minimal deficits; others need weeks to months of rehab for speech, movement, or thinking problems. Follow-up imaging and neuro visits are standard.
To lower your risk: control high blood pressure, stop smoking, limit stimulant drugs, and treat risky vascular conditions as advised by your doctor. If you or a loved one has a sudden severe headache or neurologic change, don’t wait—seek emergency care immediately.